
The follow-up time was defined as the intervals from admission to death, LT, the last clinic visit, or the end of the study on 31 December 2016. The patients were admitted for 24 h of observation following the procedure, and subsequent outpatient care was provided in an outpatient hepatology clinic. A final angiogram was performed to confirm good blood flow through the TIPS. Post-placement pressure measurements were then obtained. Postplacement dilation was carried out to 10 mm or 12 mm, as per the interventional radiologists’ preference. Gore and Associates, Flagstaff, AZ, USA) were deployed across the liver tract, followed by balloon dilation. The stent length was then measured using a marking catheter, and Viatorr covered stent grafts (W. 12 In brief, the hepatic veins were accessed via puncture of the right internal jugular vein under direct ultrasound guidance, and venography was performed to confirm hepatic venous anatomy. The technique for TIPS placement was performed according to standard clinical practice by experienced interventional radiologists under general anesthesia. 6, 11 Data also were collected on readmission for hepatic encephalopathy within 30 days after TIPS. The MELD-Na score was calculated as MELD score +1.32 × (137 − serum Na) – (0.33 × MELD score × 137 − serum Na). 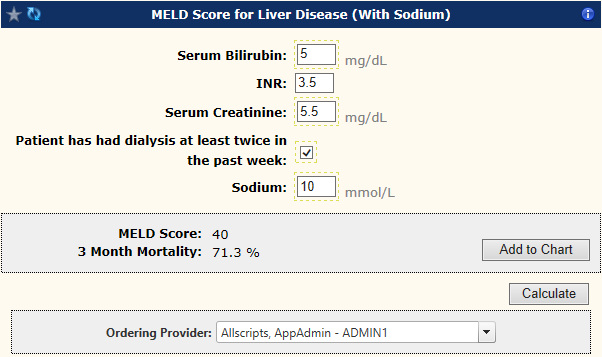
The MELD and MELD-Na scores were calculated from laboratory data obtained within 7 days before TIPS creation in accordance with previously published formulas, with the MELD score calculated as 3.78 × ln serum bilirubin level (mg/dL) + 11.2 × ln (INR) + 9.57 × ln serum creatinine (mg/dL) + 6.43. Excluded were patients who underwent TIPS after LT, TIPS for noncirrhotic portal hypertension or portal vein thrombosis, and those with lack of laboratory data prior to TIPS.ĭata on demographics, underlying liver disease, indication for TIPS, whether TIPS was considered urgent or elective, laboratory values, including serum sodium, serum creatinine, total serum bilirubin, and international normalized ratio (INR), and portosystemic gradients were collected before and after TIPS creation. Two authors manually identified all TIPS recipients to confirm that the ICD-9/10 code corresponded to a new TIPS placement. The TIPS recipients were identified using the International Classification of Diseases (ICD) code (ICD-9: 39.1, intra-abdominal venous shunt or related ICD-10 codes 06183DY and 06184DY) from Johns Hopkins electronic health records and the Johns Hopkins Interventional Radiology database for this cohort study. 5, 9, 10 We conducted this study to investigate the prognostic ability of MELD-Na compared to MELD for 30-day and 90-day mortality among patients with cirrhosis after TIPS placement. There are limited studies comparing MELD with MELD-Na for the prediction of mortality after TIPS in patients with cirrhosis, and the existing studies have conflicting conclusions. 8 Therefore, in January 2016, the MELD-sodium (MELD-Na) was implemented in place of the MELD for organ allocation in LT in the USA. It is particularly true of patients with low MELD scores, where the effect of serum sodium is significantly greater. 8, 9 Hyponatremia has been established as a key predictor of mortality in patients with cirrhosis independent of the MELD score. 6, 7 However, previous studies have shown that subgroups of patients are at a higher risk of mortality than predicted by their MELD score, thus restricting their access to LT. The model for end-stage liver disease (MELD) score was first developed to predict early death of patients undergoing elective TIPS placement and was subsequently adopted for organ allocation in candidates for liver transplantation (LT) in 2002. 3– 5 As a result, several prognostic scoring systems have been developed to assist in patient selection for TIPS placement in patients with cirrhosis. 1– 3 Careful patient selection for TIPS is vital because the resultant shunting of hepatic blood flow leads to an increased risk of post-procedure hepatic encephalopathy, liver failure, and morbidity/mortality in patients with significantly impaired liver function. The transjugular intrahepatic portosystemic shunt (TIPS) is created using percutaneous endovascular techniques to treat complications of portal hypertension such as variceal hemorrhage, refractory ascites, and hepatic hydrothorax.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
